|
|
||||||||
 |
 |
 |
||||||
 |
 |
 |
 |
 |
||||
| Sclerotherapy |
| Sclerotherapy also called as injection therapy is the oldest, simplest and the cheapest method of treating varicose veins. It has been used for over 150 years. Injection therapy is an alternate therapy used to seal varicose veins. It is most accepted and promising method of treatment as constant innovations in the technique have made it more safe and effective. It takes hardly 10 to 15 minutes for the completion of the procedure. |
| What is Sclerotherapy? |
| It is a non-surgical procedure in which a solution is injected into the varicose or spider veins in order to cause its disappearance. It is frequently used if people develop more varicose veins after surgical removal of the larger varicose veins and to seal spider-burst veins for people concerned about cosmetic appearance. Sclerotherapy is done in the office using small needles. A variety of solutions are used to do sclerotherapy and they are called as sclerosants. |
| Sodium Tetradecyl Sulfate (STS) & Polidocanol (POL) are the two most commonly used sclerosant agents. Their method of administration and the strength or dilution depends on the size of vein, the site of injection and above all the experience of the surgeon. The solution is injected at multiple sites in varying dilutions. |
| How does the Sclerosant Act? |
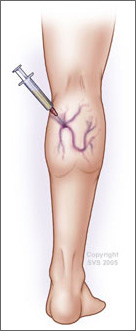 The Sclerosant produces endothelial destruction by chemical burns of the endothelium i.e. inner lining of the vein. Due to the severe inflammation of the vessel wall they stick together; vein seals shut and gets converted into a fibrotic cord. This prevents blood from entering the sealed sections of the vein. The veins remain in the body for some time, but no longer carry blood. The blood that would normally return to the heart through these veins will re-route through other normal veins and flow much more efficiently. When a problem vein is closed off after sclerotherapy, it eventually disappears by re absorption of all vascular tissue layers. The Sclerosant produces endothelial destruction by chemical burns of the endothelium i.e. inner lining of the vein. Due to the severe inflammation of the vessel wall they stick together; vein seals shut and gets converted into a fibrotic cord. This prevents blood from entering the sealed sections of the vein. The veins remain in the body for some time, but no longer carry blood. The blood that would normally return to the heart through these veins will re-route through other normal veins and flow much more efficiently. When a problem vein is closed off after sclerotherapy, it eventually disappears by re absorption of all vascular tissue layers. This procedure can be performed on an out-patient basis, no surgical incisions are made and does not require anesthesia. No hospital stay is usually required. Most patients find the treatment to have little or no pain. If at all pain at injection site is variable. In smaller veins there will be some pain but in larger veins it is practically painless. Most people need a few treatments to obtain the best results. Treatments are generally done at monthly intervals. |
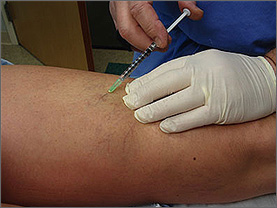 Although complications may occur with any medical treatment, sclerotherapy has a good safety record. You should always discuss the risks and treatment alternatives with your physician. The procedure has to be done by a Surgeon well experienced in the technique. Although complications may occur with any medical treatment, sclerotherapy has a good safety record. You should always discuss the risks and treatment alternatives with your physician. The procedure has to be done by a Surgeon well experienced in the technique. Your doctor may ask you not to use cream or lotion on your legs on the day of treatment. No other special preparation is needed before this therapy. During your first session, your doctor may perform a few injections to test your response to the chemical. Based on your response, the amount of the chemical may be adjusted. You may then have multiple sessions for different parts of the leg. Many veins can be treated in one session. In most cases, there is little or no pain during treatment, though you may feel a slight burning or stinging sensation. Crepe bandage is applied over the injected sites, assuring compression of veins. Compression stockings and bandages should be worn as directed by your doctor. The patient can walk about after the procedure. In fact, they should be encouraged to walk about following sclerotherapy. You may immediately return to normal activities following your procedure. However, hot environments, such as hot baths and saunas should be avoided. Walking is encouraged. Some bruising may be noticed following the procedure, but this is usually not severe. Treatment results may be seen within a few days, but it may take up to 12 weeks for treated veins to be completely reabsorbed by the body and disappear. |
| POST TREATMENT REGIMEN |
|
| In which conditions Sclerotherapy is advocated? |
| Sclerotherapy can be done in all stages of the varicose disease but usually it is reserved only for smaller and midsized veins and in cases of varicose tributaries that either persist or recur after definitive procedures for the reflux. Some centers have proved it to be very effective in larger varicose veins, including the great and short saphenous veins as well. A study by Kanter and Thibault in 1996 reported a 76% success rate at 24 months in treating SFJ and GSV incompetence with STS 3% solution. (Success rate with the CTEV: CoolTouchEndoVenous is 95 to 98%) This can be done in patients who otherwise are unfit for a definitive procedure. |
| Where not to be done? |
a. If there is Deep Vein Thrombosis |
| What are the precautions after the procedure? |
| The procedure is done preferably on one limb at a time. After the injection the patient can go home. To avoid swelling of the limbs, it is preferable to keep the limb elevated while resting. It is also advisable to use crepe bandage to the limb for at least 10 days to help the veins remain collapsed and stick together. |
| Any Side effects? |
| Side effects, if at all, are very mild. Some patients may complain of some heaviness of head, and dryness of mouth. Some may complain of itching over the injection site. In case of extravasation of fluid it can cause excruciating pain locally and subsequent tissue necrosis will develop. Allergic or Hypersensitivity reactions including Anaphylactic reactions are "extraordinarily rare but can be life-threatening," and doctors should have resuscitation equipment ready. There has been one reported case of stroke after ultrasound guided sclerotherapy when an unusually large dose of sclerosant foam was injected. Very rare chance of Deep Vein Thrombosis Local Hirsutism has been observed in a few patientsRevascularization and recanalisation of the veins contribute to recurrence. |
| Advantages |
| Very safe, very simple and economical procedure. No hospital stay. Can go back to normal activities earlier than all other techniques. Safe for very aged patients otherwise unfit for surgery. Enhanced success rate over other procedures |
| Disadvantages |
More effective only in short segments of smaller veins. Repeat sessions may be required. |
| Foam Sclerotherapy |
| The Newer technique of sclerotherapy is Foam Sclerotherapy which has got added benefits over the conventional Sclerotherapy. The overall cure rate is more than 90% in all available literature. |
| Why Foam Sclerotherapy? |
The liquid sclerosants due to gravity tends to remain only on the floor of the veins, not affecting the entire inner wall and also tends to flow away rapidly to adjacent vein segments than intended for. It also gets diluted rapidly by the blood requiring a relatively higher dose. To overcome these disadvantages, some of the sclerosants are converted into foam by agitating them with air or carbon dioxide. Here the foam rapidly displaces the blood from the vein preventing itself getting diluted, gets evenly applied to the entire inner wall of the vein. As an advantage, the dose required is less, effect is better and side effects are less. |
| Ultrasound Guided Sclerotherapy |
| Swelling or oedema of the legs is an usual feature in varicose disease. It precludes proper visualization or palpation of the veins under the skin. Extravasation of the sclerosant outside vein wall has catastrophic results. Here ultrasound comes to rescue by making these veins visible for accurate needle placement and sclerosant injection under vision. This also helps in more accurately deciding the volume of the sclerosant to be injected in the particular vein segment to avoid its passage to the deep veins through the perforators. The usual Color Doppler unit with linear probe can be used but for very small telangiectatic veins a high frequency Pencil Probe gives better picture resolution. |
Ultrasound Guided Foam Sclerotherapy Thready spider veins can be difficult to treat. Microinjection sclerotherapy with 30 gauge needle using magnification or vein visualization system is more effective than doing it without these aids. Conclusion A very safe, convenient and most cost effective procedure. Its newer techniques like foam, ultrasound guided and micro injection are promising and are likely to emerge as the best ancillary procedures to compliment the definitive closure procedures for the reflux. About Sclerosants Phenol in almond oil injected through a special cannula was the original method of Sclerotherapy. This is no more used. Sodium morrhuate is an older detergent sclerosant that is made up of a mixture of saturated and unsaturated fatty acids extracted from cod liver oil. The agent is of variable composition and has been associated with a relatively high incidence of anaphylaxis. The incidence of extravasation necrosis is high with this drug. Ethanolamine oleate, a synthetic preparation of oleic acid and ethanolamine, has weak detergent properties because its attenuated hydrophobic chain lengths make it excessively soluble and decrease its ability to denature cell surface proteins. High concentrations of the drug are necessary for effective sclerosis. Allergic reactions are uncommon, but reports exist of pneumonitis, pleural effusions, and other pulmonary symptoms following the injection of ethanolamine oleate into esophageal varices. The principal disadvantages of the drug are a high viscosity that makes injection difficult, a tendency to cause red cell hemolysis and hemoglobinuria, the occasional production of renal failure at high doses, the possibility of pulmonary complications, and a relative lack of strength compared with other available sclerosants. |
Hypertonic sodium chloride solution in a 20% or 23.4% solution can be used as a sclerosing agent. The principal advantage of the agent is the fact that it is a naturally occurring bodily substance with no molecular toxicity, but the disadvantages of the agent make it unsuitable except in the hands of highly skilled practitioners.
|
| Sodium Tetradecyl Sulfate (STS) & Polidocanol (POL) are the currently used agents and both are known as detergent sclerosants because they are amphiphilic substances that are inactive in dilute solution but are biologically active when they form micelles. These agents are preferred because they have a low incidence of allergic reactions, produce a low incidence of staining and other cutaneous adverse effects, and are relatively forgiving if extravasated. |
| Effective Sclerotherapy |
A high degree of technical skill is necessary for effective sclerotherapy for the following reasons:
|
|
||||
 |
|
|||||||||||
|
|
|
|
|
|
|
|
|
|
|
||